- +1 (773) 985-1869
- info@stream-rcm.com
- 14430 Ocean Point, El Paso, TX 79938
Stream RCM delivers inclusive healthcare revenue cycle management in medical billing for practices, physicians, and healthcare organizations to manage the full RCM lifecycle from patient intake and claim submission to denials resolution and final reimbursement. Minimize denials, boost cash flow, and strengthen financial performance.













Best Medical Billing believes that doctors and nurses shouldn’t have to chase reimbursements. That’s why our medical billing service providers champion even the most complex medical coding claims to drive the most accurate healthcare insurance reimbursement rates for every physician that uses our end-to-
end health revenue cycle management services.
That’s why our medical billing service providers champion even the most complex medical coding claims to drive the most accurate healthcare insurance reimbursement rates for every physician that uses our end-to- end health revenue cycle management services.
Advanced imaging to visualize blood vessels with high clarity. Helps diagnose blockages, narrowing, and circulation problems
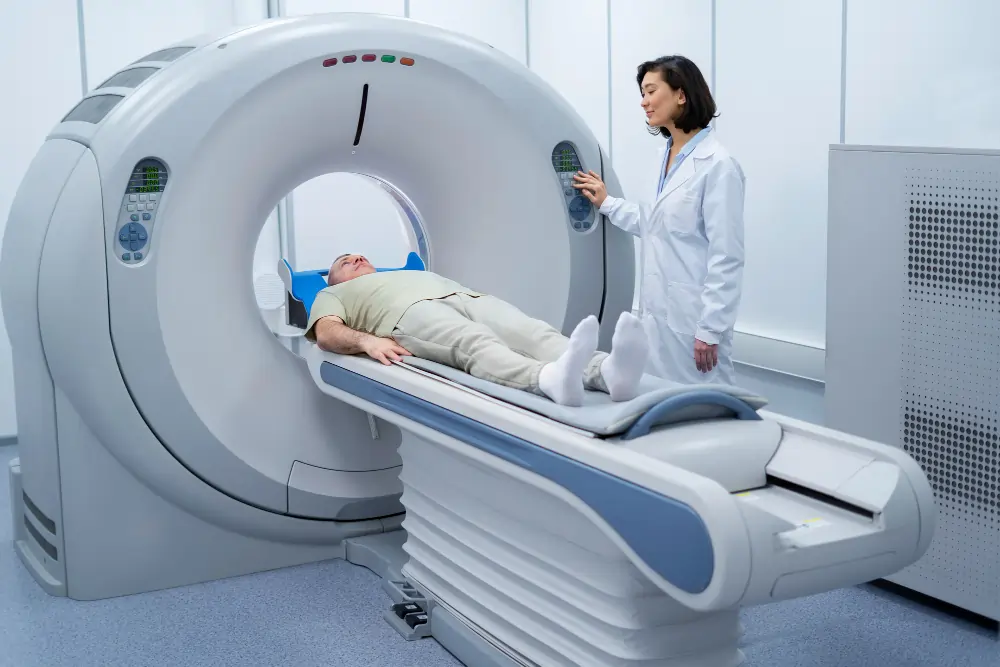
Accurate testink to monitor and analyze your heart’s electrical activity Melos detect arrhytamios and early cardiac abnormalities.

Accurate testink to monitor and analyze your heart’s electrical activity Melos detect arrhytamios and early cardiac abnormalities.

Accurate testink to monitor and analyze your heart’s electrical activity Melos detect arrhytamios and early cardiac abnormalities.

Accurate testink to monitor and analyze your heart’s electrical activity Melos detect arrhytamios and early cardiac abnormalities.

We work by connecting you with skilled virtual assistants in just four easy steps. With us, you can simplify your workflow in a hassle-free way!
Full revenue cycle management for urology practices from cystoscopies and biopsies to urodynamics and vasectomies.
Full revenue cycle management for urology practices from cystoscopies and biopsies to urodynamics and vasectomies.
Full revenue cycle management for urology practices from cystoscopies and biopsies to urodynamics and vasectomies.
Full revenue cycle management for urology practices from cystoscopies and biopsies to urodynamics and vasectomies.
Full revenue cycle management for urology practices from cystoscopies and biopsies to urodynamics and vasectomies.
Full revenue cycle management for urology practices from cystoscopies and biopsies to urodynamics and vasectomies
We deliver scalable, HIPAA-compliant cardiology billing solutions focused on accurate coding, complete charge capture, and proactive denial management to maximize reimbursements.

Effective pain management billing processes need sophisticated financial infrastructures that are able to cope with intricate coding systems, changing insurance policies, and procedures-driven billing methods. Stream RCM provides expert pain management medical billing services for physicians that surpass those of regular in-house billing systems due to automation technology, certification in coding, and specialty-oriented billing strategies. This method improves payment accuracies, reduces waste in operations, and shields pain management practices from risks of non-compliance. By integrating insurance information, denial analyses, and account management, Stream RCM allows physicians to attain sustainable financial performance without any distractions from their patients.
They rely on manual processes that cause inconsistent and inefficiencies of financial outcomes which are often unpredictable.
They rely on manual processes that cause inconsistent and inefficiencies of financial outcomes which are often unpredictable.
They rely on manual processes that cause inconsistent and inefficiencies of financial outcomes which are often unpredictable.
They rely on manual processes that cause inconsistent and inefficiencies of financial outcomes which are often unpredictable.
They rely on manual processes that cause inconsistent and inefficiencies of financial outcomes which are often unpredictable.
They rely on manual processes that cause inconsistent and inefficiencies of financial outcomes which are often unpredictable.
They rely on manual processes that cause inconsistent and inefficiencies of financial outcomes which are often unpredictable.
They rely on manual processes that cause inconsistent and inefficiencies of financial outcomes which are often unpredictable.
They rely on manual processes that cause inconsistent and inefficiencies of financial outcomes which are often unpredictable.
They rely on manual processes that cause inconsistent and inefficiencies of financial outcomes which are often unpredictable.
Stream RCM is the top affordable medical billing company in the USA, with more than 15 years of experience helping healthcare providers, clinics, hospitals, and doctors to improve their revenue cycle and overall financial performance. We work with hospitals and medical practices to accurately generate, submit, and follow up on claims, as well as pay claims, manage denials, and collect funds. We do not only convert medical data into billable claims; rather, we manage the entire billing process accurately and transparently, providing complete revenue cycle management for more than 50 medical specialties.

Modernize clinical workflows with your existing healthcare systems to improve workflow efficiency and data consistency.


Stream RCM is an affordable medical billing service provider that offers billing services to medical practices to improve claim submission, denial reduction, compliance, cash flow, practice revenue, with a high success rate of 99.9% first-pass acceptance.
While cardiologists focus on saving lives, Stream RCM handles the billing challenges that protect revenue and keep practices thriving
Constant CPT & ICD changes that silently disrupt billing accuracy and revenue flow
We run continuous code validation workflows and real-time updates so your claims never rely on outdated or deleted codes.
Advanced procedures under payer review leading to audits and claim rejection risks
Our team builds claims with audit-level accuracy, aligning documentation, modifiers and medical necessity to reduce payer scrutiny on complex procedures like cath labs and EP studies.
Documentation gaps that fail to fully justify and support the billed medical services
We bridge the gap between clinical notes and billing requirements, ensuring every claim clearly proves medical necessity.
Missed revenue from undercoding or incomplete charge capture
We identify hidden revenue opportunities by reviewing encounters line-by-line because even small coding gaps can cost practices tens of thousands annually.
Payer-specific rules, prior authorization, and inconsistent reimbursement policies
Our workflow adapts to each payer’s logic, reducing rework and preventing denials caused by authorization and policy mismatches.
Denials that accumulate over time and remain unresolved, causing ongoing revenue loss
We actively track, appeal, and resolve denials because a large percentage of denied claims are never resubmitted, leading to avoidable revenue loss.
We work by connecting you with skilled virtual assistants in just four easy steps. With us, you can simplify your workflow in a hassle-free way!

Simply schedule a meeting with us to begin the process. We’ll discuss your business needs and how we can assist woul
Simply schedule a meeting with us to begin the process. We’ll discuss your business needs and how we can assist woul
Simply schedule a meeting with us to begin the process. We’ll discuss your business needs and how we can assist woul
Simply schedule a meeting with us to begin the process. We’ll discuss your business needs and how we can assist woul
Medical billing refers to filing claims about healthcare to the insurers to be reimbursed. It makes sure that the providers are paid on time, stay in line with the regulations, minimize the denials, avoid revenue losses, and stay financially stable by the smooth organization of administrative mechanisms.
Medical coding uses services that are assigned standardized codes such as ICD-10, CPT and HCPCS. Proper coding leads to claim acceptance, optimal reimbursement, avoiding claim denials, negative compliance risks and appropriate documentation to back up insurance payments.
Clean claims usually require 15-30 days to get reimbursement based on the insurer. Delays are brought about by errors, incomplete information or even denials. Professional billing services will make submission faster, unpaid claims are followed and will result in speedy and uniform payments.
We cover behavioral health, family practice, gastroenterology, optometry, urgent care, general surgery and long-term care. Our customized billing systems accommodate the specialty needs of practices, facilitating the enhancement of efficiency, accuracy, compliance, and revenue at practices.
The denied claims are analyzed to find out the problem with coding, documentation, or eligibility, fix and resubmit timely. Our proactive follow up on insurers helps us to reduce delays, recover revenue, reduce repeat denials and to ensure constant cash flow.

Improve collections, reduce outstanding invoices, and accelerate cash flow with expert-led AR follow-up services.